from Leadership Medica n. 9/2005
Introduction
Strabismus is a frequent disease in children (3-5% incidence). Normal eye position is called orthophoria
or orthotropia. Strabismus is such a severe lack of eye alignment that makes binocular vision impossible.
It can be:
horizontal
- convergent or esotropia
- divergent or exotropia.
vertical
hypertropia (Fig. 1)
hypotropia.
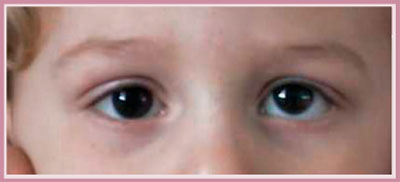
Convergent strabismus counts 80% of eye deviations with 65% of unilateral deviations, which always effect the same eye, and 35% of alternating deviations, which affect both one eye and the contralateral
one.
Strabismus is defined concomitant when the deviation is identical in all eye positions and incomitant when the deviation is greater in a certain eye position, as occurs in paralytic strabismus.
Esotropia can be distinguished in 3 groups:
- early onset,
- late onset,
- microstrabismus
Exotropia or divergent strabismus can be either constant or intermittent.
The intermittent form has the best prognosis because stereoscopic vision is preserved. Exodeviations, which appear at a very early stage and with a high angle, are frequently found in children with collicerebral lesions in infancy.
Generally strabismus’ early onset - especially if it is unilateral - can be a sign of eye disease (cataract, retinoblastoma, chorioretinal scars or other congenital diseases). Strabismus associates motor signs with important sensory signs and symptoms. The most relevant of these are: suppression, amblyopia and abnormal retinal correspondence.
Amblyopia is a visual deficit, whose severity can vary. This sign is the most important one to be recognised and treated when associated with strabismus.
Diagnostic evaluation
The cross-eyed patient’s examination involves:
- inspection and observation of the position of the head
- study of eye motility in the nine eye positions corneal reflexes
- cover test to define the presence of deviation
- measurement of the deviation visual field examination
- refraction in cycloplegia
- examination of the anterior segment and of the fundus oculi
Corneal Reflexes
They exploit the cornea’s mirroring features. The penlight stimulus pointed before the eyes is placed symmetrically in the centre of the pupil in orthophoric patients. A shifted reflection with reference to the centre and its asymmetry are a sign of deviation.(fig.2)
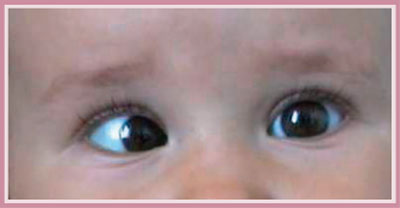
Cover test
The apparently staring eye is covered to evaluate the behaviour both of the same eye and of the contralateral one when the screen is removed. No movement is appreciated in conditions of orthotropia.
In cases of unilateral strabismic deviation, the deviated eye straightens when the apparently staring eye is covered, but it returns to the strabismic position when the screen is removed.
In cases of alternating deviation, when the apparently staring eye is covered the contralateral one straightens and maintains the position after the screen is removed.
4 Dioptre Vision Test
A 4 dioptre prism placed before the eye of normal individuals enables to observe the behaviour of the contralateral eye, which first has a rapid movement towards the apex of the prism and a second slow returning movement. In cases of microstrabismus no movement is observed when a prism is placed before the eye that is not staring. (fig.3)

Refraction
The refraction test must always be performed after cycloplegia through the administration of colliria such as cyclopentolate, which is currently the most frequently used one. Some authors prefer to use 1% tropicamide.
Atropine is currently reserved to certain cases. The examination, which evaluates the presence of refractive defects is called sciascopy.
In collaborative patients sciascopy, which remains the main test, is currently combined with autorefractometry, which is a computerised detection method of refraction.
Sight defects are hypermetropia, myopia and astigmatism.
Either associated with astigmatism or not, hypermetropia is the most common defect that has been found in convergent strabismus.
Myopia is more frequently associated with divergent strabismus.
The correction of the visual defect when strabismus is present must be complete and consider the values found in cycloplegia.
Examination of the anterior segment and of the fundus oculi The evaluation of the anterior segment by means of a slit lamp and the examination of the fundus oculi complete the eye examination and are necessary to rule out eye diseases as a cause of strabismus.
 Fig. 4, 5, 6 - Teller's Card for visual acuity in babies 6 month/1 years age
Fig. 4, 5, 6 - Teller's Card for visual acuity in babies 6 month/1 years age
Treatment principal
Medical Treatment
The first treatment envisages complete optical correction of the defect in refraction with permanent lenses. When amblyopia is present the choice treatment is occlusion of a variable duration depending on the patient’s age. (fig. 7)
 Fig. 7 - Occlusion
Fig. 7 - Occlusion
The occlusion must not be passive but active (games or work for near sight), both to achieve better patient compliance and to obtain satisfactory results in a shorter time. The maintenance treatment after occlusion makes use of penalising methods such as the use of filters applied to lenses. The use of adequately built bifocal lenses is recommended in the forms characterised by excessive convergence (high AC/A ratio). (Fig. 8)
 Fig. 8 - Bifocal lenses for incomitance far/near
Fig. 8 - Bifocal lenses for incomitance far/near
Surgical Treatment
The end of surgical treatment is both functional and aesthetical. Surgical treatment is the final action in the diagnostic-rehabilitative course of strabismic patients who require a repeated series of tests and examinations. Surgery must possibly be recommended when there is alternating strabismus and equal vision in both eyes. Surgical treatment aims at removing the visual axes’ relative deviations. Surgery is performed on eye muscles to influence the very muscles’ activity and subsequently eye alignment. Operations are hence distinguished either in surgery focused either on weakening muscle action (withdrawal) or on strengthening it (resection).
The choice of the type and extent of surgery depends on the assessment of eye motility, on the characteristics of the deviation and on the measurement of the same. Let us now study some special cases of strabismus.
Essential infantile esotropia
Strabismus with an early onset (essential infantile esotropia) sets in during the first 4-6 months of life: parents often notice the deviation at birth. This deviation is characterised by:
- large deviation angle (often more than 50 dioptres)
- crossed fixation
- abduction deficit (due to the lateral rectal muscle’s failure to contract) latent nystagmus
- ocular stiff neck (not always present)
- mild hypermetropia (rarely high)
- hyperfunction of the mall oblique muscles (it can be noticed after the child’s 1st year) (Fig. 9)
- dissociated vertical deviation (to be distinguished from the hyperfunction of the small oblique muscles).
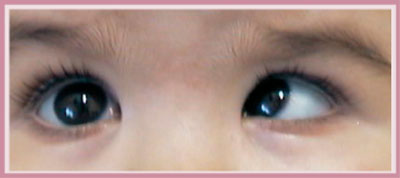 Fig. 9 - Esohypertropia
Fig. 9 - Esohypertropia
Diagnosis
When there is strabismus an eye examination must be performed as soon as possible to highlight the presence of sensory anomalies, the most important of which is amblyopia (sight deficit due to lack of use). When amblyopia is present early treatment is essential to obtain good results and the total recovery of sight.
Treatment
correction of the refractive defect occlusion traditional surgery (withdrawal of the median rectal muscles either associated or not with the withdrawal of the small oblique muscles).
Botulinum toxin treatment has been recently used as an alternative to traditional surgery.
The injection is administered to the median rectal muscles according to a well coded method within the child’s 7th – 8th month of life. Literature has reported satisfactory results in terms of eye alignment (60-70%). (fig.10 e fig.11)
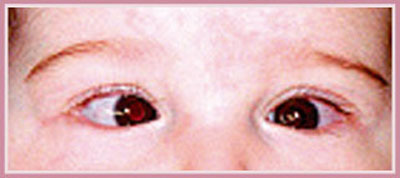
Fig. 10 - Esotropia pre-toxine
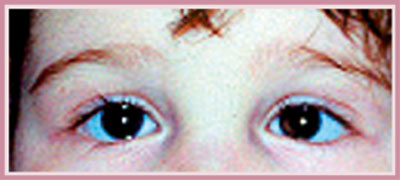
Fig. 11 - Esotropia post-toxine
Non refractive accomodative esotropia
High AC/A ratio
It is another form of accommodative esotropia, which cannot be corrected with lenses used for hypermetropia. In this case the patient is orthophoric at distant sight and esotropic at near sight when the correction is applied. These patients respond very well to bifocal lenses, which must be adequately produced to ensure that the section of the lens corresponds to the centre of the pupil.
Microstrabismus
It is strabismus with a small strabismic deviation, which parents find hard to detect. Hence the diagnosis can be delayed. Microstrabismus must be suspected when there is a small unilateral visus.
It is characterised by:
|
- anisopia
- amblyopia - eccentric fixation - abnormal retinal correspondence - lack of stereoscopic perception. |
Diagnosis
4 prism dioptre test (lack of the refixation reflex when the prism is placed before the deviated eye).
Treatment
Correction of a refractive defect.
Occlusion.
Exotropia
This term defines divergent strabismus.
Exodeviations are less frequent than esodeviations with a 1:4 ratio.
Classification:
basic exotropia
excessive divergence
convergence deficit.
Forms resulting from excessive divergence have a greater deviation with distance sight rather than near sight. Inadequate convergence has a greater deviation for near sight rather than distant sight. Exotropia can either be intermittent or constant
Intermittent exotropia
Intermittent exotropia is a condition which alternates periods of deviation control with periods of decompensation. A typical feature of deviation is the closing of one eye when the patient is outdoors and in brightly lit environments.
Treatment of Exotropia
Spherical negative lenses can improve deviation control especially in exophoria/ tropia and in intermittent forms. Orthoptic exercises improve the visual field but they cannot substitute surgery. The recommendation to perform surgery generally considers the type of exotropia: inadequate convergence with high deviation angles requires resection of the median rectal muscles.
Alphabetic attitudes
Alphabetic syndromes are conditions in which horizontal deviation changes when one shifts from a downward stare to an upward stare. It is called syndrome A when maximum convergence occurs upwards, while it is called syndrome V when the maximum convergence is downwards. An esotropia in A will have a maximum horizontal deviation with the upward stare and a minimum horizontal deviation with the downward stare. An esotropia in V will have the maximum deviation with the downward stare and the minimum horizontal deviation with the upward stare.
The opposite occurs with exotropia.
These attitudes can be associated with an abnormal position of the head (i.e. chin turned upwards or downwards to maintain the position in which the eyes are most aligned).
In case of esotropia in V associated with an oblique muscle dysfunction, the procedure envisages withdrawal of the same.
In cases which present a slight alphabetic attitude, vertical movements of the horizontal rectal muscles can be implemented along with withdrawal of the median rectal muscles.
The rule is to move the median rectal muscles towards the apex of A or V and vice versa the lateral rectal muscles.
Conclusions
Strabismus is an important disease, which requires special dedication and commitment both on the part of the specialist and the patient.
Since the disease has a higher incidence in children, the treatment requires frequent and careful control of the visual function to enable the appropriate and symmetrical development of the two eyes’ visual acuity. Early recognition also enabled by growing collaboration with the paediatrician is doubtless a good starting point to achieve the best results.
Surgical treatment must be considered the final action in this diagnostic-therapeutic course designed to achieve an eye alignment that is closest to orthophoria, keeping in mind that surgical correction’s primary goal is not the aesthetical aspect, but the functional one of reestablishing binocular cooperation.


Dr.ssa E. Piozzi, Dr.ssa A. Del Longo
Paediatric Ophthalmology, Niguarda
Ca' Granda Hospital, Milan



