da Leadership Medica n. 1 del 2001
Abstract
Authors make a survey of Anderson-Fabry disease, first appeared at the end of nineteenth century. Genetical causes, main clinical manifestations, different treatment: results of the activity of an experienced group of nephrologists.
Article
 Anderson-Fabry disease (AF), or the familial deficiency disorder of a-galactosidase A, is caused by a congenital error in the glycosphingolipid metabolism that derives from a defect in the activity of a lysosomal hydrolase: the enzyme a-galactosidase A. It has been documented that this enzymatic error is transmitted by a gene made up of seven hexones, present on the long arm of the X chromosome in the region q 21,22.
Anderson-Fabry disease (AF), or the familial deficiency disorder of a-galactosidase A, is caused by a congenital error in the glycosphingolipid metabolism that derives from a defect in the activity of a lysosomal hydrolase: the enzyme a-galactosidase A. It has been documented that this enzymatic error is transmitted by a gene made up of seven hexones, present on the long arm of the X chromosome in the region q 21,22.
This enzymatic defect involves the progressive accumulation of neutral glycosphingolipids, with an alphagalactosidic terminal tract, i.e. a cerebroside di- and trihexoxide, in most of the body’s fluids and tissues.
This accumulation of neutral glycosphingolipids occurs inside the lysosomes of the endothelial cells, epithelial cells, smooth muscle cells, myocardial and kidney cells, and in the cells of the reticuloendothelial system, connective tissue, corneal epithelium, nerve ganglia and the perineural cells of the autonomic nervous system. In 1898, a British dermatologist called W. Anderson published in the British Journal of Dermatology the clinical case of a male patient aged 39 years who presented with diffused angiokeratomas with a clear presence of proteins in the urine. Anderson put forward his suspicion that the patient did not simply have a skin disorder, but was presenting with a systematic disease, and that the anomalies of the capillaries, which he had observed in the skin, might also be present in the renal capillaries.
In the same year, and even contemporaneously and without being aware of W. Anderson’s paper, the German dermatologist J. Fabry published in the Archives Von Dermatologie und Siphilis journal, the clinical case of a 13 year-old male that presented with extensive angiokeratoma, albumin in the urine, and small arteriolar aneurysms. It took until 1955 to see the first American report on a rare disorder, Fabry’s disease, published in Archives of Internal Medicine. In 1967, Brandy demonstrated that the enzymatic defect resided in trihexosidase ceramide, a galactosyl hydrolase contained in the lysosomes of cellular cytoplasm. Subsequently, the enzymatic defect in Anderson-Fabry disease was precisely identified in the a-galactosidase A. The clinical manifestations depend on the presence of organ lesions, and are expressed more completely and severely in males, hemizygotes, than in females, heterozygotes, at times totally asymptomatic. The clinical pictures observed and described in AF disease patients are characteristically very polymorphic for reasons that are still not definite, and perhaps related to the nature and site of the genetic error. AF disease is classified among the major sphingolipidoses (Tab. I) and is considered a rare disorder, having an incidence rate of 1:40,000, although it is probably more widespread that what is commonly thought, such that it has been suggested that the plasma level of a-galactosidase A be carried out in all those patients that have arrived at a terminal uremia without a safely ascertained diagnosis.

Clinical manifestations
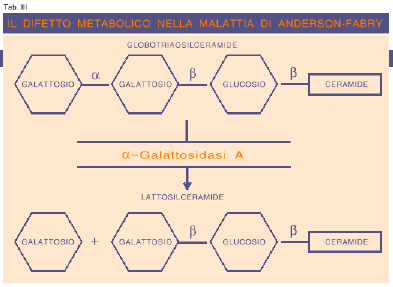
The clinical manifestations of AF disease (set out in Tab. II) are very heterogeneous and represent the anatomic and physiological sequelae of the pathological progressive accumulation of the trihexoxide galactosyl-galactosyl-glucosyl-ceramide within the lysosomes of cells belonging to various organs and apparatus. In physiological conditions, a-galactosidase A determines the breakdown of globotriaosylceramide into lactosylceramide (Tab. III), which is removed by the reticuloendothelial system. The shortage of enzyme leads to the pathological cellular accumulation of the trihexoxide, histologically documentable in organs before there are clear clinical signs of the disease.

Neurological
Painful paroxysmal crises in the extremities (considered secondary to lesions of the dorsal radices of the ganglioneures) are generally the onset manifestation of the disease in childhood or early adolescence. The crises, generally precipitated by intense exercise or emotive stress, last from a few minutes to some days and tend to be contained as regards intensity and frequency with getting older. In addition to the crises some patients complain of persistent acroparesthesias. However, 10-20% of elderly AF disease carriers deny any history of painful crises or acroparesthesia. Cerebrovascular manifestations, possible in this disorder’s more advanced stages, are the outcome of a multifocal impairment in the microcirculation. RMN evaluation is the test of choice for revealing lacunar lesions of the central nervous system. Other neurological signs: intestinal dismotility and altered vasomotility due to involvement of the autonomic nervous system, dementia, and personality disturbances.
Dermatological
Although atypical variants of this disease have been described without cutaneous involvement, the angiokeratomas with a characteristic “swimming costume” distribution (symmetrical involvement of the lower trunk, perineum and scrotum) may represent the disorder’s earliest manifestation and generally consent to the diagnosis already in the childhood age range. A careful examination of the skin is necessary where the disease is suspected, in order to detect isolated skin lesions not evident on a routine objective assessment.
Oculistic
“Verticillated cornea” is a typical dystrophic corneal lesion occurring in 100% of the hemizygote males and 70% of the female heterozygotes. This alteration may only be detected by means of a split-lamp ophthalmoscopic examination. Vascular lesions of the retina and conjunctiva are common in the context of a systemic vascular involvement.
Cardiological
The cardiac pathology is very polymorphic:
- electrocardiogram PR interval abbreviation is common, and in the past was considered characteristic in AF disease patients;
- histological alterations in the conduction system responsible for atrioventricular block have been documented at autopsy;
- The high incidence of cardiac arrhythmia and in particular atrial fibrillation in the juvenile age range is known;
- Coronary artery disorders can be very severe, and are often the cause of death;
- The incidence of valvular anomalies is very common and mitral prolapse is present in 50% of the hemizygote patients, although usually not hemodynamically significant;
- Left ventricular hypertrophy is a common finding and has been reported as the only alteration in an atypical variant in hemizygote subjects, in the absence of valvulopathies and arterial hypertension.
The complexity and variability of the cardiac clinical manifestations are correlated to the patient’s age and sex, and are attributable to the progressive accumulation of globotriaosylceramide in the heart’s various structures. Electron microscope studies on myocardial biopsies permits a definitive diagnosis to be made.
Nephrological
Renal clinical manifestations are also increasingly evident in hemizygote males compared to the heterozygote females, according to the Lyon hypothesis, unless in the latter the mutated X chromosome prevails over the normal one. The kidneys appear bigger because of the ceramide accumulation in every tract of the nephron, and in every cellular strain present I the kidney, as well as in the vascular endothelium. Since the glycosphingolipid accumulation is especially in the epithelium of Henle’s loop and the distal tubule, the capacity for concentration is soon impaired. The tubular dysfunction can be more complex and also involve the proximal tubule with aminoaciduria, normoglycemic glycosuria and renal tubular acidosis as in Fanconi syndrome. The proteinuria may be isolated, without alteration of the urinary sediment, and appears in juveniles. Progression towards terminal chronic renal failure is the most common complication in male patients.
Diagnosis
The nephrological involvement of AF disease derives from the possibility of diagnosis by means of an ultrastructural examination of the kidney biopsy that documents typical cytoplamic inclusions, present in all the cellular strains of the nephron. This is a matter of small osmiophilic, ovoidal bodies having diameters between 1-3m, laminated concentrically due to the alternating of the electron-dense laminae and electron-lucent spaces. With optical microscopy it is possible to suspect AF disease by the aspect of the epithelium of the renal tubular structures characterised by abnormal accumulated material; immunofluorescence is not significant. The study of urinary sediment by electron microscope can be diagnostic (Fig. 1). The diagnosis is confirmed in the finding of reduced enzymatic activity by a-galactosidase A both in the plasma and in peripheral leukocytes. 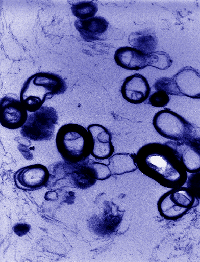 Testing for plasma cerebroside trihexoxide levels documents its increase and is accompanied by high urinary levels to the extent that the glomerular filtrate is maintained within normal limits. It is opportune to advise testing for a plasma deficiency of the lysosomal hydrolase a-galactosidase A, just as for a rise in plasma and urine levels of the cerebroside trihexoxide, in all the proband’s consanguineal family members whether male or female. It would also be useful to extend the research with thorough dermatological and oculistic consultations, and with an echocardiograph check. The technique for the patients’ DNA restriction polymorphisms can give a genetic diagnostic confirmation and can lead to identifying the kind of genetic mutation that characterises the proband and his/her family relations. Pre-natal diagnosis of AF disease can be made by means of amniocentesis already by the 14th week of gestation, recognising the XY karyotype on the culture of amniotic cells and detecting a shortage of a-galactosidase A, or else with trophoblast DNA analysis of the chorial villi on a biopsy sample.
Testing for plasma cerebroside trihexoxide levels documents its increase and is accompanied by high urinary levels to the extent that the glomerular filtrate is maintained within normal limits. It is opportune to advise testing for a plasma deficiency of the lysosomal hydrolase a-galactosidase A, just as for a rise in plasma and urine levels of the cerebroside trihexoxide, in all the proband’s consanguineal family members whether male or female. It would also be useful to extend the research with thorough dermatological and oculistic consultations, and with an echocardiograph check. The technique for the patients’ DNA restriction polymorphisms can give a genetic diagnostic confirmation and can lead to identifying the kind of genetic mutation that characterises the proband and his/her family relations. Pre-natal diagnosis of AF disease can be made by means of amniocentesis already by the 14th week of gestation, recognising the XY karyotype on the culture of amniotic cells and detecting a shortage of a-galactosidase A, or else with trophoblast DNA analysis of the chorial villi on a biopsy sample.
Therapy
At the moment there is no specific therapy. The use of steroids is suggested for controlling painful symptoms. Since increased platelet aggregation and a high plasma level of b-tromboglobulin have been observed, long-term treatment with ticlopidine and vitamin E has been proposed, with the purpose of preventing possible thromboembolic complications. The terminal chronic uremia patient should be treated with the usual dialysis techniques and with kidney transplantation that, however, does not make up for the enzyme shortage. The current therapeutic prospect is the use of the a-galactosidase A enzyme. A recent study would demonstrate the effectiveness and manageability of the IV infusion of the lacking enzyme derived from the culture of human fibroblasts. The single infusion of the purified enzyme (well tolerated in the 10 patients comprising the study) determined a significant reduction in the liver, plasma and urine levels of the globotriaosylceramide substrate. The long histic half-life allows its weekly or fortnightly administration. A grand hope, therefore, of being able to control this invalidating hereditary disease in a substantial and definitive way.
Dott. Adalberto Sessa
Primario di Nefrologia e Dialisi - Ospedale di Vimercate
Bibliografia
Sessa A, Meroni M, Battini G : Eterogeneità fenotipica della malattia di Fabry: malattia rara?. Giornale Italiano di Nefrolgia 1997; vol.14 n.4:195-201
Meroni M., Sessa A, Battini G, Tazzari S, Torri Tarelli L: Kidney involvement in Anderson-Fabry disease. Contrib to Nephrol 1997; vol 122:178-184 Eng
C.M, Resnick D.J, Silverman L.A, Niehaus D.J, Astrin K.H, Desnick R.J : Nature and frequency of mutations in the a-galactosidase A activity gene that cause Fabry disease. A. J. Hum genet 1993; vol 53:1186-1197
Desnick R.J, Joannou Y.A, Eng C.M: a-galactosidase A deficiency Fabry disease. The metabolic and molecular bases of inherited disease. 7th ed New York:Mc Graw Hill 1995:2741-2784
Meroni M, Spini C, Tazzari S, Sessa A, et al: Isolated glomerular proteinuria as the only clinical manifestation of Fabry’s disease in an adult male. Nephrol Dial Trasnsplant 1997; vol 12:221-223
Nakao S, Takenaka T, Maeda M, Kodama C. et al: An atypical variant of Fabry’s disease in men with left ventricular hypertrophy. NEJM 1995; vol 333:288-293
Chimenti C, Ricci R, Pieroni M, Natale L, Russo M, Frustaci A : Cardiac variant of Fabry’s disease mimiching hypertrophic cardiomyopathy. Cardiologia 1999; vol 44:469-473
Shiffmann R, et al: Infusion of a-galactosidase A reduces tissue globotriaosylceramide storage in patients with Fabry’s disease. PNAS 2000;vol 97:365-370



