from Leadership Medica n. 1/2002
 The aspect of the ovary is an essential sign of the Polycystic Ovary Syndrome (PCOS), which is also associated with a number of biochemical disorders, such as high plasmatic concentrations of androgynous LH, insulin and a reduced sensitivity to insulin action. Patients suffering from ovarian polycystosis are often overweight. Since insulinoresistance in female patients is prevalently an extra-splanchnic phenomenon, glycaemia values usually remain normal. The above-mentioned symptoms are usually displayed in approximately 10% of women; therefore the Polycystic Ovary Syndrome appears to be the most frequent endocrine disorder affecting young women. Whilst the presence of an anomalous ovary morphology is highly prevalent (over 20%), the clinical signs may be poor and, more specifically, there is no evidence of a systematic negative effect of polycystosis on fertility; indeed, a controlled study conducted on female patients subject to in-vitro fertilization did not detect significant differences between the rate of pregnancies induced in normal women and in patients suffering from the syndrome in question (Mac Dougall et al., 1993). However, other studies have reported a significant prevalence of both primary and secondary sterility; a high rate of miscarriages has also been reported in conjunction with PCOS, in patients with high circulating LH values. In view of the high rate of affected patients, it is many years now that researches suspect that this syndrome has a genetic basis. This hypothesis was analysed during several studies on the PCOS phenotype in different populations.
The aspect of the ovary is an essential sign of the Polycystic Ovary Syndrome (PCOS), which is also associated with a number of biochemical disorders, such as high plasmatic concentrations of androgynous LH, insulin and a reduced sensitivity to insulin action. Patients suffering from ovarian polycystosis are often overweight. Since insulinoresistance in female patients is prevalently an extra-splanchnic phenomenon, glycaemia values usually remain normal. The above-mentioned symptoms are usually displayed in approximately 10% of women; therefore the Polycystic Ovary Syndrome appears to be the most frequent endocrine disorder affecting young women. Whilst the presence of an anomalous ovary morphology is highly prevalent (over 20%), the clinical signs may be poor and, more specifically, there is no evidence of a systematic negative effect of polycystosis on fertility; indeed, a controlled study conducted on female patients subject to in-vitro fertilization did not detect significant differences between the rate of pregnancies induced in normal women and in patients suffering from the syndrome in question (Mac Dougall et al., 1993). However, other studies have reported a significant prevalence of both primary and secondary sterility; a high rate of miscarriages has also been reported in conjunction with PCOS, in patients with high circulating LH values. In view of the high rate of affected patients, it is many years now that researches suspect that this syndrome has a genetic basis. This hypothesis was analysed during several studies on the PCOS phenotype in different populations.
Studies Conducted on Different Races
A research conducted in California (Carmina et al., 1992) analysed 75 patients suffering from ovarian polycystosis and coming from three different ethnic groups and found that, whilst the obesity and hirsutism values varied depending on environmental factors, the various ethnic groups displayed a uniform impact with respect to excessive production of androgens and insulinoresistance. However, more recent studies have demonstrated that the ethnicity and PCOS phenotype factors act as independent deficiencies displaying a cumulative effect in influencing insulin activity.
A recent study suggests that the PCOS phenotype represents a major risk factor, versus ethnic group or race, owing to the reduced tolerance to glucose (Legro et al., 1999).
Studies on Twins
The Polycystic Ovary Syndrome has occasionally been reported in monozygotic twins. An Australian study has proved the impact of PCOS on both sisters in 34 couples of twins. On the other hand, the high degree of variance in the ovary sonographic image detected between twin sisters, suggests a complex hereditary transmission and/or a major role of environmental factors, capable of altering the expression of the genetic signal. The authors themselves, in order to offer an explanation as to the high prevalence of the Polycystic Ovary Syndrome in twin sisters, have suggested the existence of factors capable of acting during intrauterine life (Jahnfar et al., 1995).
Studies on PCOS Families
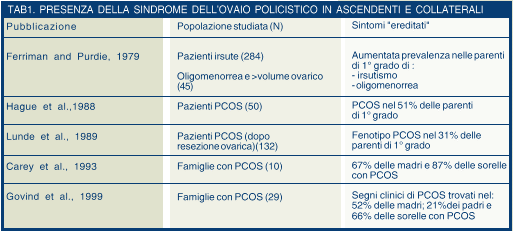
The polycystic aspect of the ovary, menstrual irregularities and insulinoresistance are the symptoms that have been taken into account in the various studies investigating family transmission of the syndrome. On the other hand, the only somatic feature reported for the male subjects involved was early baldness. The studies reported in Table 1 display a significant prevalence of PCOS in the patients’ female relatives in the 1st degree. Two accurate studies on the presence of the syndrome in ascendants and collaterals both suggest that hereditary PCOS is transmitted according to a dominant autosomal model (Franks et al., 1997; Govind et al., 1999).
Mechanisms of Hereditary Transmission
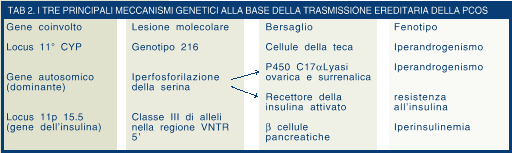
A) Hyperandrogynism
1 – Excessive Ovary Activity
In patients suffering from polycystosis, the cells of the ovarian theca produce an excessive amount of progesterone and of androgens. This factor led to the study of the behaviour of the gene responsible for the detachment of the cholesterol lateral chain (CYP 11a) as a possible cause of the anomalous steroidogenesis. Therefore, in 1997, Gharani and his team, by studying the segregation of this gene in patients suffering from PCOS, were able to assess that its most common polymorphism (indicated as 216-) is associated with the syndrome. The non-parametric linkage analysis performed in this region of the genoma confirmed that gene CYP11a is the true cause of the genetic liability of this type of hyperandrogynism displayed by many patients suffering from ovarian polycystosis.
2 – Excessive Ovary and Adrenal Gland Activity
The excessive production of androgens by patients suffering from PCOS may also be ascribed to the enzymatic activity accomplished by the cytochrome P450 C17a. The hyperphosphorylation of serine in the enzyme molecule significantly stimulates steroidogenetic activity, both at an ovary and at an adrenal level, by causing an increase in the production of androgens without however affecting the ACTH levels (Zhang et al., 1995).
B) Insulinoresistance
Insulinoresistance certainly represents another frequent metabolic factor displayed by patients suffering from Polycystic Ovary Syndrome. The metabolic disorder may be related to a reduced functionality of the insulin receptor, which is again aided by a hyperphosphorylation of the serine residues by the receptor. Indeed, its excessive phosphorylation reduces the endocrine signal of the hormone, thus leading to an insulinoresistance situation (Holte, 1996). Therefore, in other words, the hyperphosphorylation mechanism, which as regards the cytochrome P450 C17 induces ovarian and adrenal hyperandrogynism, by altering the activity of the insulin receptor, may also be deemed to be responsible for insulinoresistance. A single molecular deficiency may therefore explain two of the chief disorders characterising the syndrome associated with ovarian polycystosis.
C) Hyperinsulinemia
Excessive production of insulin by the pancreas is often displayed by patients suffering from polycystic ovaries and is reported to be one of the most serious risk factors as regards the future development of non-insulin-dependent diabetes. The excessive incretory activity of the beta-cells does not depend on obesity and in most PCOS patients is not associated with a reduced intolerance to glucose. Some recent studies have investigated the behaviour of the gene that regulates the incretion of insulin in patients suffering from PCOS. It has thus been found that in the VNTR5" region of the gene for insulin, a connection exists between class III alleles and the PCOS condition (Bennet et al., 1995). The same result emerged from a linkage analysis conducted on families displaying PCOS heredity. It was therefore concluded that the VNTR5" region of the insulin secretion gene represents a location responsible for the hyperinsulinemia associated with the Polycystic Ovary Syndrome (Waterworth et al., 1997).
PCOS : Environmental Factors
A) Prenatal Factors
In 1997 Cresswell and his team investigated the features of pregnancies leading to the birth of women who later developed PCOS. The authors were therefore able to divide the patients affected by ovarian polycystosis into two groups. The 1st group included subjects who were overweight at time of birth ad had obese mothers, whereas the 2nd group included subjects whose weight was normal at time of birth, but who were born beyond the physiological pregnancy time limit. Based on these observations, the authors postulated that during intrauterine life there are two factors capable of favouring the development of postnatal PCOS: the mother’s obesity and/or high weight at time of birth may indeed be responsible for the excessive ovarian production of androgens and for postnatal obesity; on the other hand, in PCOS patients who had a normal weight at time of birth, but were born after an extended pregnancy, this situation could involve a defective control over LH secretion during adult life.
B) Postnatal Factors
- Anovulation
A causative role of chronic anovulation in the Polycystic Ovary Syndrome is suggested by the various physiopathologic mechanisms involving the secretion of LH, of androgens and the hepatic production of SHBG.
- Obesity
Obesity is an independent risk factor for chronic anovulation and a “central” distribution of fat appears to be more significant than over-weight itself, (Zaadstra et al., 1993). In obese women, the two chief mechanisms responsible for anovulation are the same that are activated by the Polycystic Ovary Syndrome:
- excessive secretion of LH and androgens;
- hyperinsulinemia and insulinoresistance.
Between the two endocrine mechanisms strong links exist. Indeed, fasting, even only over a short period, reduces the secretion of LH in ordinary weight women (Olson et al., 1995). In overweight patients, caloric restrictions reduce the levels of circulating insulin and increase the concentrations of SHBG (Kiddy et al., 1992). In patients suffering from serious obesity, the recovery of ordinary weight following gastroplasty normalises the glycaemia and insulinemia values. On the contrary, in patients suffering from PCOS, obesity worsens the syndrome. In particular, insulinoresistance appears to be linked to the body mass index, whereas ponderal reduction in obese patients suffering from ovarian polycystosis reduces LH hyperincretion and restores a normal sensitivity to insulin. Experimental data also suggest the existence of genetically controlled mechanisms capable of modifying the sense of appetite, body weight perception and the reproductive function.
(trad. Interpres sas Giussano)
Piergiorgio Crosignani
Direttore del Dipartimento Ostetricia e Ginecologia I.C.P Milano
Bibliografia
1) Bennet S.T., Lucassen A.M., Gough S.C.L., Powell E.E., Undlien D.E. Protchard L.E., Merriman M.E., Kawaguchi Y., Dronsfield M.J., Pociot F., et al., (1995), “Susceptibility to human type 1 diabetes at IDDM2 is determined by tandem repeat variation at the insulin gene minisatellite locus.” Nat. Gen., 9:284-92.
2) Carey A.H., Chan K.L., Short F., White D., Williamson R., Franks S. (1993) “Evidence for a single gene effect in polycystic ovaries and male pattern baldness.” Clin. Endocrinol. 38: 653-8.
3) Carmina E., Koyama T., Chang L., Stanczyk F.Z., Lobo R.A., (1992) “Does ethnicity influence the prevalence of adrenal hyperandrogenism and insulin resistance in polycystic ovary syndrome ?” Am. J. Obstet. Gynecol., 167:1807-12. Cresswell J.L., Barker D.J.P., Osmond C., Egger P., Phillips D.I.W., Fraser R.B. (1997) “Fetal growth, length of gestation, and polycystic ovaries in adult life.” Lancet, 350:1131-5.
4) Ferriman D., Purdie A.W. (1979) “The inheritance of polycystic ovarian disease and a possible relationship to premature balding.” Clin. Endocrinol., 11: 291-300.
5) Franks S., Gharani N., Waterworth D., Batty S., White D., Williamson R., McCarthy M. (1997) “The genetic basis of polycystic ovary syndrome.” Hum. Reprod.,12:2641-8.
6) Friedman J.M. (1997) “The alphabet of weight control.” Nature, 385:119-20.
7) Gharani N., Waterworth D.M., Batty S., White D., Gilling-Smith C., Conway G.S., McCarthy M., Franks S., Williamson R. (1997) “Association of the steroid synthesis gene CYP11a with polycystic ovary syndrome and hyperandrogenism.” Hum. Mol. Genet., 6:397-402.
8) Govind A., Obhrai M.S., Clayton R.N. (1999) „Polycystic ovaries are inherited as an autosomal dominant trait: analysis 29 polycystic ovary syndrome and 10 control families.“ J. Clin. Endocrinol. Metab., 84: 38-43.
9) Hague W.M., Adams J., Reeders S.T., Peto T.E., Jacobs H.S. (1988) “Familial polycystic ovaries: a genetic disease?” Clin. Endocrinol. (Oxf), 29;: 593-605.
10) Holte J. (1996) “Disturbances in insulin secretion and sensitivity in women with the polycystic ovary syndrome.” Clin. Endocrinol. Metab., 10:221-47.
11) Jahnfar S., Eden J.Z., Warren P., Seppala M., Hgyun T.V. (1995) “A twin study of polycystic ovary syndrome.” Fertil. Steril., 61:478-86.
12) Kiddy D.S., Hamilton-Farley D., Bush A., Short F., Anyaoku V., Reed M.J., Franks A.D. (1992) “Improvement in endocrine and ovarian function during dietary treatment of obese women with polycystic ovary syndrome.” Clin. Endocrinol. Oxf., 36:105-11.
13) Legro R.S., Kunselman A.R., Dodson W.C., Dunaif A. (1999) “Prevalence and predictors of risk for type 2 diabetes mellitus and impaired glucose tolerance in polycystic ovary syndrome: a prospective, controlled study in 254 affected women.” J. Clin. Endocrinol. Metab., 84: 165-169.
14) Lunde O., Magnus P., Sandvik L., Hoglo S. (1989) “Familial clustering in the polycystic ovarian syndrome.” Gynecol. Obstet. Invest., 28: 23-30.
15) Mac Dougall M.J., Tan S.L., Balen A., Jacobs H.S. (1993) “A controlled study comparing patients with and without polycystic ovaries undergoing in-vitro fertilization.” Hum. Reprod., 8:233-7.
16) Olson B.R., Cartledge T., Sebring N., Defensor R., Nieman L. (1995) “Short-term fasting affects luteinizing hormone secretory dynamics but not reproductive function in normal-weight sedentary women.” J. Clin. Endocrinol. Metab., 80:1187-93.
17) Waterworth D.M., Bennett S.T., Gharani N., McCarthy M.I., Hague S., Batty S., Conway G.S., White D., Todd J.A., Franks S., Williamson R. (1997) “Linkage and association of insulin gene VNTR regulatory polymorphism with polycystic ovary syndrome.” Lancet, 349:986-90.
18) Zaadstra B.M., Seidell J.C., Van Noord P.A., te Velde E.R., Habbema J.D., Vrieswijk B., Karbaat J. (1993) “Fat and female fecundity: prospective study of effect of body fat distribution on conception rates.” Br. Med. J., 306:484-7.
19) Zhang L.H., Rodriguez H., Ohno S., Miller W.L. (1995) “Serine phosphorylation of human P450c17 increases 17,20-lyase activity: implications for adrenarche and the polycystic ovary syndrome.” Proc. Natl. Acad. Sci. USA, 92:10619-23.



