from Leadership Medica n. 2/2006
Abstract
Benign pancreatic hyperenzymemia is a new syndrome recently described by me and characterized by an abnormal increase in serum pancreatic enzymes in the absence of pancreatic disease. Hyperenzymemia can be sporadic or familial, it involves all the pancreatic enzymes and is persistent, although the values fluctuate considerably even temporarily returning to normal levels.
Recognition of this syndrome is very important as it helps to reassure subjects
with this anomaly, usually very concerned, that the syndrome is benign and that no pancreatic diseases are present; it also helps to avoid the need to carry out numerous examinations and sometimes also hospitalization and treatments that are completely
useless.
Summary:
- Introduction
- Phatological pancreatic hyperenzymemia
- Nonpathological pancreatic hyperenzymemias
- Studies by other authors on benign pancreatic hyperenzymemia
- Association of benign pancreatic hyperenzymemia and nonpathological serum increases of other compounds
- Final Considerations
- Bibliography
Introduction
In 1986 I first saw a 46-year-old man, in excellent health, who had had abnormally high serum pancreatic enzymes for several months. He had been admitted to my department for suspected pancreatic disease but all the biohumoral and imaging techniques carried out, including wirsungography, were normal. I thought that the hyperenzymemia could be the expression of a
pancreatic disease (chronic pancreatitis? tumor?) that was still not evident but which would have emerged in the days or months that followed. Instead, no pancreatic disease ever became apparent, the patient continued to enjoy good health in the years that followed and still does, his
serum pancreatic enzymes are frequently high and imaging techniques show an
absolutely normal pancreas. Since then, I have seen numerous other subjects, children and adults, with the same enzymatic anomaly, and with a normal pancreas1,2. In this article, I will describe the main characteristics of this new syndrome.
Phatological pancreatic hyperenzymemia
There are many forms of pancreatic hyperenzymemia and they may be pathological and non-pathological; the most frequent forms are pathological and, in particular, are caused by diseases of the pancreas (Table 1).
In general, an increase in the normal serum values of pancreatic enzymes is due to the presence of acute pancreatitis, but even chronic pancreatitis, especially during the painful attacks or when complicated by pseudocysts, tumors and pancreatic trauma can also cause hyperenzymemia.
Pancreatic hyperenzymemia can also sometimes be encountered in other diseases, mainly cystic fibrosis, celiac disease, intestinal infarct or perforation, renal insufficiency, kidney transplant, hepatitis and cirrhosis of the liver, chronic intestinal inflammatory diseases, and acute pancreatic
ischemia after surgery involving the heart or the aorta, especially the thoracic aorta3. These forms of hyperenzymemia are usually easy to recognize and their identification can be of considerable diagnostic help. In addition to these forms, there is also a vast group of non-pathological pancreatic hyperenzymemias (Table 1).
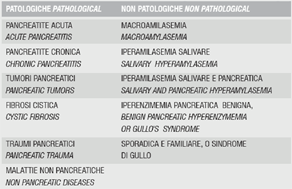 Table 1: pancreatic hyperenzymemia
Table 1: pancreatic hyperenzymemia
Nonpathological pancreatic hyperenzymemias
Hyperamylasemia
This form of hyperenzymemia has been well-known for many years. An increase in just the serum values of amylase can be found in healthy subjects in various conditions, in the absence of pancreatic diseases4-7. This group includes hyperamylasemia due to the presence of macroamylase, salivary hyperamylasemia and mixed, salivary and pancreatic, hyperamylasemia. Macroamylase is a macrocomplex consisting of normal serum amylase bound to an abnormal serum protein; this macrocomplex accumulates in the circulation as it is too large to be filtered by the renal glomerulus and causes hyperamylasemia. Salivary hyperamylasemia is due to an increase in the serum of the amylase produced by the salivary glands, while the mixed form is caused by an increase of both the salivary and pancreatic enzyme in the circulation. A simple criterion for distinguishing macroamylasemia from the other two forms of hyperamylasemia is the dosage of amylasuria, which is normal when hyperamylasemia is due to macroamylase and increased in the other two forms. Two studies published in 19978 and 20029 described cases of familial hyperamylasemia. Each study described just one subject with hyperamylasemia, reporting that the enzymatic defect was also present in some of the patient's relatives. Both patients, however, suffered from recurrent abdominal pain, which casts some doubt on the complete absence of any disease of the pancreas.
Benign pancreatic hyperenzymemia or Gullo's syndrome
This is a new form of pancreatic hyperenzymemia which I described for the first time, characterized by an abnormal increase in the serum of all pancreatic enzymes.
There is a sporadic form1 and a familial form2. In the first study dedicated to this anomaly1, I described the sporadic form in 18 subjects, seen between January 1987 and June 1991 (10 males and 8 females, mean age 47 years, range 25-66). The interval between the initial detection of hyperenzymemia and the start of the study varied from 4 months to 10 years, with a mean value of 12.6 months. These were all normal subjects, in excellent health and without any disease. At the time of the study they underwent various examinations, including ultrasound, CT and/or wirsungography. After the initial observation they were clinically followed until December 1995. The pancreatic hyperenzymemia had been discovered during routine tests which had also by chance included amylase. Figure 1 shows the individual serum values of amylase, isoamylase, lipase and trypsin detected at the time of the study. As can be seen, the enzymes were abnormally high in all subjects. The increase above the upper limit of the normal range varied from 1.4 to 4.1 times for amylase, from 1.8 to 6.0 times for pancreatic isoamylase, from 1.5 to 7.7 times for lipase and from 1.6 to 13.9 times for trypsin. During the subsequent follow-up which lasted for around five years,the enzymes remained high, albeit with considerably fluctuating values and sometimes returning to within the normal range, as shown in figures 2 and 3 which report the serum enzyme levels of two cases followed for nine years. Neither of the 18 subjects studied has presented any signs or symptoms of pancreatic disease in the years that followed the study. In a subsequent study2. I described the familial form of this benign pancreatic hyperenzymemia, a form that involves more than one member of the same family. In this study, I reported seven families in which two or more members, making a total of 19 subjects (11 males and 8 females; mean age, 32.7 years; range 3- 84), had this enzymatic defect. None of these 19 subjects had signs or symptoms of pancreatic disease; routine blood tests and abdominal ultrasound scans were normal in all of them.
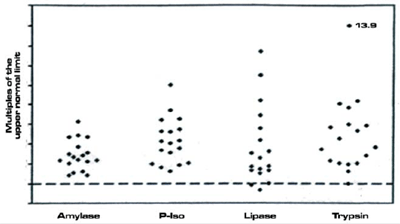 Figure 1
Figure 1
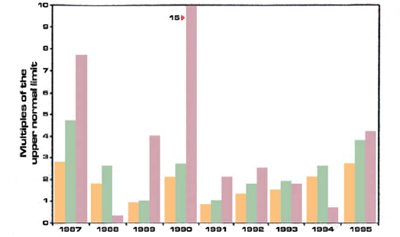
Figure 2
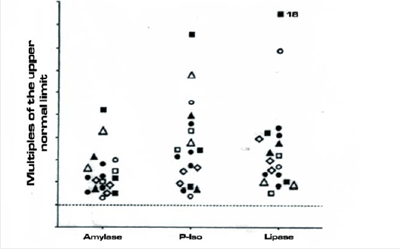
Figure 3
Figure 3 shows the serum values of amylase, isoamylase and lipase in the 19 subjects at the time of the study. It can be seen that the enzymes were higher than normal, with increases ranging from 1.3 to 5.2 times the upper normal limit for amylase, from 1.4 to 8.6 times for pancreatic isoamylase and from 1.6 to 18.0 times for lipase. The determination of the serum pancreatic enzymes was repeated over the following months and years and the results were similar, with fluctuations and transient normalizations. The members of the seven families affected by hyperenzymemia were a mother, her two sisters and two daughters; a mother and her two children; a father and two children; three fathers and their respective three children, and one brother and sister. Overall, there were five children under the age of 10 years.
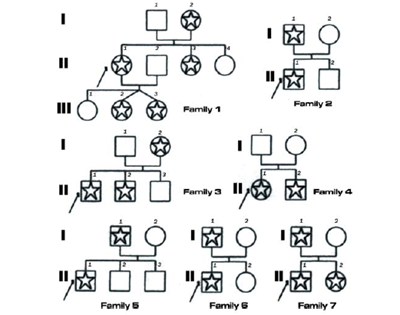 Figure 4
Figure 4
Figure 4 shows the family tree of the seven families; the carriers of the enzymatic alteration are indicated with a star.
In a subsequent study10 we found that in subjects with this form of hyperenzymemia the administration of secretin, a hormone that stimulates pancreatic secretion, leads to a marked increase of serum pancreatic enzymes, especially lipase. This suggests that the abnormal secretion of circulating enzymes occurs not only in basal conditions but also after hormonal stimulation. The underlying mechanism of this abnormal passage of enzymes from the
pancreatic cell into the blood is unknown. The fact that the defect has been detected in more than one member of the same family indicates the possibility of a genetic basis. In a study which has been recently published11 we evaluated whether mutations of the cystic fibrosis gene (CFTR, cystic fibrosis transmembrane regulator) may play a role in the etiology of this form of hyperenzymemia. The results showed that only seven of the 70 subjects studied had mutations of this gene; this frequency is similar to that is found in the general population and the result does not therefore support a role of CFTR gene mutations in the etiology of this form of pancreatic hyperenzymemia. In another paper, currently in press12, we decided to study whether pancreatic hyperenzymemia remains constant or whether it varies over a number of days. We therefore measured serum pancreatic enzymes for five consecutive days in a vast group of subjects affected by this new syndrome. We found that in most cases the hyperenzymemia is not constant, and the values can vary from one day to the next, at times even returning to within the normal range.
Figure 5 shows the values for one of these cases. The reason for these frequent variations is unknown.
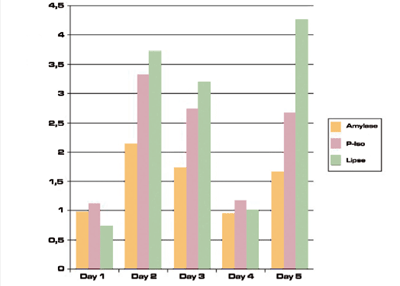 Figura 5
Figura 5
Studies by other authors on benign pancreatic hyperenzymemia
Very few studies have been published on this topic. In a letter to the editor which appeared after my first article on the syndrome1, some authors13 claimed that the hyperenzymemia could be caused by pancreatic steatosis, secondary to a condition of hypercholesterolemia and/or hypertriglyceridemia present in some of the subjects affected by the enzymatic abnormality.
The diagnosis of pancreatic steatosis had been made with ultrasound. Apart from the fact that pancreatic steatosis has never been described in humans, a study of the pancreas which we performed in a group of subjects with hyperenzymemia and increased cholesterol and/or triglycerides using magnetic resonance, which clearly reveals the presence of any pancreatic fatty infiltration, unmistakably showed that the pancreas was normal and free of any fatty infiltration12. In another letter to the editor following my first study1, a group of Spanish authors14 reported five cases of sporadic pancreatic hyperenzymemia similar to those which I had described and confirmed my results. Finally, I recall a study that was published in 199115 reporting three cases of hyperamylasemia and hyperlipasemia without apparent causes. The authors concluded that, although subclinical pancreatic damage could not be excluded, the finding still had an indeterminate clinical significance. One of the three subjects had in fact formerly had acute pancreatitis and another was a heavy drinker, making it difficult to claim the absence of possible causes of the hyperenzymemia, at least in these two cases.
Association of benign pancreatic hyperenzymemia and nonpathological serum increases of other compounds
Benign serum increases of other compounds have been known for many years to exist. The first of these to be reported was the increase in unconjugated bilirubin or Gilbert's syndrome (16), clinically characterized by mild and intermittent jaundice. Another benign increase was first reported in 1980 by Rowland et al (17) who described the possibility of nonpathological serum increases of creatine phosphokinase (CK), which was confirmed more recently in other studies (18, 19). In some of the subjects with benign pancreatic hyperenzymemia I have found an association with Gilbert's syndrome or with an increase in creatine phosphokinase. In others, I have found an association with a nonconstant and nonpathological increase in transaminases
(20). Whether these associations are casual or have a common genesis is not clear.
Final Considerations
The following considerations should be bornein mind for correct recognition ofbenign pancreatic hyperenzymemia:
1.This form of hyperenzymemia appears in healthy subjects, it persists over time with considerable fluctuations, often returning to within the normal range and there is no clinical or morphological evidence of pancreatic disease; it may be sporadic or familial.
2. At least a year must pass after the first finding of hyperenzymemia before it can be considered with sufficient certainty to be this new syndrome. It is important to remember that, although a very rare occurrence (1-2%), isolated pancreatic hyperenzymemia, especially in subjects over the age
of 50-60, can be the first clinical sign of a tumor of the pancreas which does not become evident for several months.
3. In almost all cases (~95%) the serum levels of all the pancreatic enzymes are abnormally high; sometimes (~5% of cases) there is only an increase in amylase or, even more rarely, in only lipase.
4. The correct diagnosis of this form of hyperenzymemia is very important as it reassures the carriers of this enzymatic abnormality, usually very concerned, that they do not have a disease of the pancreas and it avoids often numerous tests, and sometimes hospitalisation and treatment,
that are of no use whatsoever.
Lucio Gullo
Director of the “Istituto di Medicina Interna,
Università di Bologna, Ospedale S. Orsola”
Bologna, Italy
1. Gullo L. Chronic nonpathological hyperamylasemia of pancreatic origin. Gastroenterology 1996; 110: 1905-1908.
2. Gullo L. Familial pancreatic hyperenzymemia.Pancreas 2000; 20: 158-160.
3. Gullo L, Cavicchi L, Tomassetti P,Spagnolo C, Freyrie A, D'Addato M. Effects of ischemia on the human pancreas. Gastroenterology 1996; 111: 1033-1038.
4. Berk JE, Kizu H, Wilding P, Searcy RL. Macroamylasemia: a newly recognized cause for elevated serum amylase activity. N Engl J Med 1967; 277: 941-946.
5. Warshaw AL, Lee KH. Macroamylasemia and other chronic nonspecific hyperamylasemias:
chemical oddities or clinical entities? Am J Surg 1978; 135: 488-493.
6. Levitt MD, Ellis CJ, Meier PB. Extrapancreatic origin of chronic unexplained hyperamylasemia.
N Engl J Med 1980; 302: 670-671.
7. Warshaw AL, Hawboldt MM. Puzzling persistent hyperamylasemia, probably neither pancreatic nor pathologic. Am J Surg 1988; 155: 453-456.
8. Cuckow PM, Foo AY, Jamal A, Stringer MD. Familial hyperamylasaemia. Gut 1997; 40: 689-690.
9. Koda YKL, Vidolin E. Familial hyperamylasemia. Rev Hosp Clin Med S Paulo 2002; 57: 77-82.
10. Gullo L, Ventrucci M, Barakat B, Migliori M, Tomassetti P, Pezzilli R. Effect of secretin on serum pancreatic enymes and on the Wirsung duct in chronic nonpathological pancreatic hyperenzymemia. Pancreatology 2003; 3: 191-194.
11. Gullo L, Mantovani V, Manca M, Migliori M, Bastagli L, Pezzilli R. Mutations of the CFTR gene in idiopathic pancreatic hyperenzymemia.Pancreas 2005; 31: 350-352.
12. Gullo L, Manca M, Migliori M, Calculli L,Bastagli L, Salizzoni E. Pancreatic hyperenzymemia
and dyslipidemia: a study of the pancreas by magnetic resonance and evaluation of the diurnal variations of serum pancreatic enzymes. (In publication).
13. Cavallini G, Frulloni L, Vaona B, Di Francesco V, Bovo P. Is hyperamylasemia related to dyslipidemia?Gastroenterology 1997; 112: 1058 (Letter to the Editor).
14. Martinez J, Gomez A, Palazon JM, Gutierrez A, Perez-Mateo M. Asymptomatic chronic hyperamilasemia of unknown origin: an infrequent entity? Gastroenterology 1997;112: 1057 (Letter to the Editor).
15. Ventrucci M, Pezzilli R, Festi D. Clinical significance of chronic hyperamylasemia.Dig Dis Sci 1991; 36: 1517-1522.
16. Gilbert A, Leerboullet P. La cholémie simple familiale. Sem Med Paris 1901; 21: 241-243.
17. Rowland LP, Willner J, Cerri C, Di Mauro S, Miranda A. Approaches to the membrane
theory of Duchenne muscular dystrophy. In: Angelini C, Danieli GA, Fontanari D (eds). Muscular dystrophy research: advances end new trends. Excerpta Medica, Amsterdam. 1980, pp 3-13.
18. Uncini A, Papasso M, Di Muzio A. IperCKemia asintomatica: ruolo dell'indagine neurofisiologica. Neurol Sci 2001; 22: S581-S583.
19. Prelle A, et al. Retrospective study of a large population of patients with asymptomatic or minimally symptomatic raised serum creatine kinase levels. J Neurol 2002; 249: 305-311.
20. Gullo L, Migliori M, Tomassetti P, Steinberg W. Pancreatic hyperenzymaemia and hypertransaminasaemia in healthy subjects. Report of three cases. Dig Liv Dis 2003; 35: 58-60.



